Cornea Keratoconus
- Home
- Eye Care Services
- Cornea Keratoconus
Cornea Cross-Linking
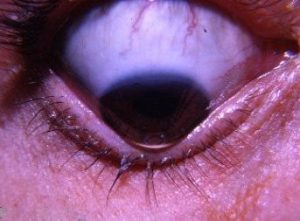 Keratoconus is an eye condition where the cornea thins and causes a distortion to its surface.
Keratoconus is an eye condition where the cornea thins and causes a distortion to its surface.
Nearly 90% of the cornea is made of overlaid collagen fibrils that are interconnected with cross-links to give the cornea strength and stability. When the cornea distorts in shape, patients complain of poor vision – notably, nighttime haloes and streaks.
There are a number of options to improve vision but none of them stops the disease from progressing. In some patients, this means that there is a need for a corneal transplant. The results are variable and patients still need to wear glasses or contact lenses. Furthermore, complete healing can take more than a year. In order to maintain the health of the graft, long-term eye drops are also required.
In order to reduce the likelihood of corneal transplant surgery, it is advisable to consider corneal cross-linking treatment. Cross-linking treatment aims to prevent the progression of keratoconus. However, it will not reverse the distortion.
Once the eye is numbed with drops, further drops of Riboflavin are added to the eye. Riboflavin is instilled until the cornea is saturated. A small dose of UV-A light is used to activate the Riboflavin. This increases the number of cross-links, resulting in a strengthened cornea. Cross linking is the sensible option for patients with mild to moderate progressive keratoconus.
DSEK
Over time, the cornea in some individuals can become hazy because of injury or slowly progressing disease. This haziness occurs because of damage to a thin, delicate layer of cells in the cornea, called the endothelium. As a result, vision becomes hazy and blurred.
Previously, the only treatment option was to transplant the entire thickness of the cornea. Modern surgical techniques only remove the damaged layer of the cornea. Known as DSEK, or Descemet’s Stripping Endothelial Keratoplasty, this technique has significantly reduced recovery times and improved vision, compared to conventional corneal transplant surgery.
The procedure involves gently removing the thin damaged layer out of the eye. The donor tissue is folded and inserted into the eye. An air bubble is then used to carefully unfold the donor tissue. The air bubble helps to secure the donor tissue to the eye.
Initially, vision will be blurred. However, as the bubble absorbs, vision will improve significantly. In some cases, the donor tissue can loosen and detach. In this case, the bubble will need to be re-applied in order to re-attach the donor tissue to the eye.
ICRS Suitability
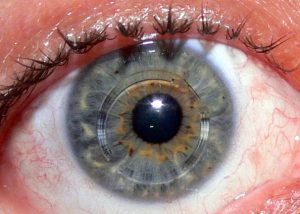 The irregular shape of the cornea in keratoconus causes a distortion to vision, especially at night.
The irregular shape of the cornea in keratoconus causes a distortion to vision, especially at night.
The intracorneal rings surgical procedure is designed to improve vision in patients with keratoconus where glasses and contact lenses are no longer tolerated. Intracorneal rings can also postpone the need for a corneal transplant. Once the rings are implanted, they are virtually invisible to the naked eye.
ICRS Treatment
The intracorneal ring procedure involves placing thin, clear, semi-circular, plastic rings into the cornea. The rings are carefully placed inside an opening less than 2mm wide, inside the cornea. Vision is improved by making the shape of the cornea more regular. The degree of shape change is controlled by the thickness of the rings. Intracorneal rings are barely visible to the naked eye and can be removed if the need arises. Ask about intracorneal rings for improved comfort and clearer vision with contact lenses.
Topography
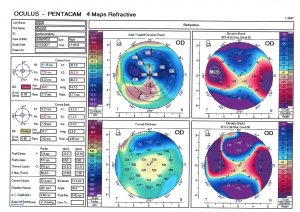 Corneal topography is an advanced technology to measure the shape of the cornea. Modern-day topographers can measure thousands of points in the cornea, resulting in an ultra-high definition assessment of its profile. Corneal topography measurement is painless and takes less than a minute.
Corneal topography is an advanced technology to measure the shape of the cornea. Modern-day topographers can measure thousands of points in the cornea, resulting in an ultra-high definition assessment of its profile. Corneal topography measurement is painless and takes less than a minute.
As the cornea is the most powerful optical component of the eye, any changes to its shape can adversely affect vision. Advanced computer calculations provide your practitioner with colour-coded maps that inform your practitioner about the presence of conditions like keratoconus, where the cornea becomes an irregular shape. Corneal topography is invaluable during complex contact lenses fitting to better align the lens with the shape of the eye. Furthermore, anyone having any form of laser eye surgery, such as LASIK or PRK, will be required to have a topography scan before and after the procedure.
Transplant
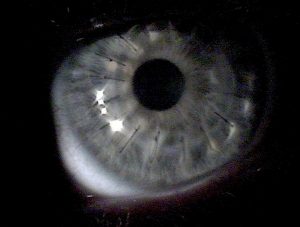 A corneal transplant involves the removal of the damaged cornea and replacing it with a donor cornea. Modern-day corneal transplantation has evolved significantly. If only the top layers of the cornea are damaged, your surgeon will transplant only the upper layers. This results in lower rejection rates, improved stability, and better vision. Your surgeon can perform a procedure called DSEK, where this thin layer is removed and replaced with donor tissue. Unfortunately, in some cases, the entire cornea may need to be replaced with a full thickness corneal graft.
A corneal transplant involves the removal of the damaged cornea and replacing it with a donor cornea. Modern-day corneal transplantation has evolved significantly. If only the top layers of the cornea are damaged, your surgeon will transplant only the upper layers. This results in lower rejection rates, improved stability, and better vision. Your surgeon can perform a procedure called DSEK, where this thin layer is removed and replaced with donor tissue. Unfortunately, in some cases, the entire cornea may need to be replaced with a full thickness corneal graft.